Palliative Care vs Hospice: A Clear Side-by-Side Guide for Families Making Decisions This Spring
Spring often brings a fresh look at what matters most—comfort, time together, and making plans that reduce stress for everyone involved. If your family is facing serious illness, you may be comparing palliative care vs hospice and wondering which type of support fits best right now.
Here’s a clear, side-by-side guide to help you make a confident decision—plus practical questions to ask and examples of what care can look like at home.
What palliative care and hospice have in common
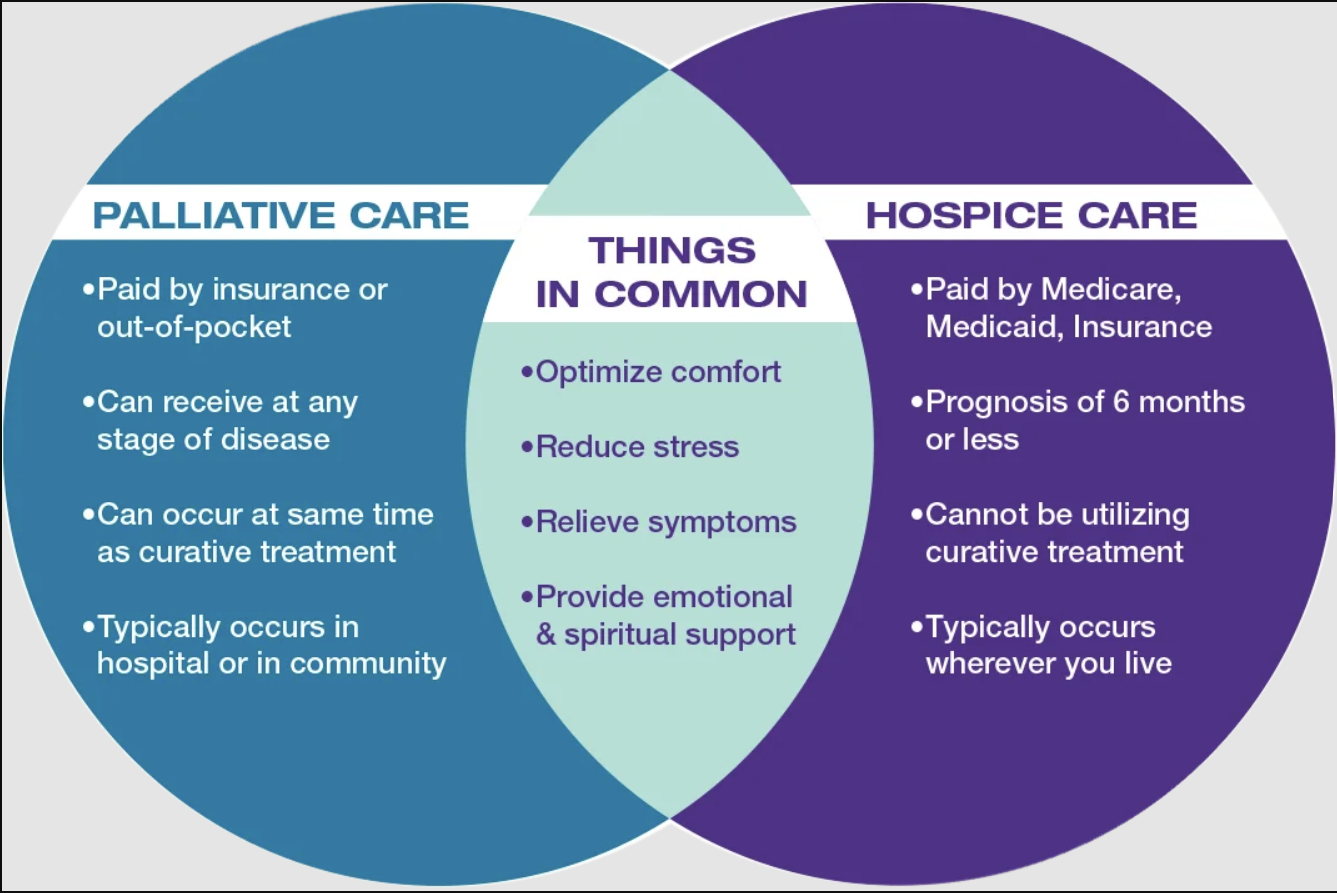
Both models are built around comfort and quality of life, not “giving up.” Whether you’re weighing palliative care vs hospice care or simply trying to understand options, these shared foundations can help:
- Symptom relief: pain, shortness of breath, nausea, fatigue, anxiety, insomnia, and more.
- Whole-person support: medical, emotional, and practical help for both patient and family.
- Team-based care: often includes nurses, physicians, social workers, chaplains/spiritual support, and aides.
- Family education: what to expect, how to manage symptoms, and how to make day-to-day care more manageable.
A helpful mindset shift
Instead of thinking “Which one is better?” ask: Which level of support matches our needs this season—right now? Many families begin with palliative care and transition to hospice later when eligibility and goals align.
Palliative care vs hospice: the side-by-side differences families need
When families search palliative care vs hospice, they’re usually trying to clarify three key issues: timing, goals, and how care is delivered.
Eligibility and timing
- Palliative care: available at any stage of a serious illness and can be provided alongside curative or life-prolonging treatment.
- Hospice care: generally available when a physician believes life expectancy may be six months or less if the illness follows its usual course, and the focus shifts away from curative treatment.
Example:
- A person undergoing chemotherapy who struggles with nausea, pain, and anxiety may benefit from palliative care support.
- A person with advanced heart failure who has frequent hospitalizations and wants comfort-focused care at home may be ready for hospice care.
Goals of care
- Palliative care: focuses on improving daily life while you pursue treatments you still want.
- Hospice care: focuses on comfort, dignity, and support—often at home—when the priority is quality of life.
If you’re looking for a deeper overview of what hospice includes, visit our page on hospice care: https://www.transitionshc.com/hospice-care
Where care happens
- Palliative care: may be offered in hospitals, outpatient clinics, or sometimes at home, depending on local availability.
- Hospice care: commonly provided wherever the patient lives—home, assisted living, or a nursing facility.
What services are included
Hospice commonly provides a more comprehensive home-based support structure. Depending on needs, this can include:
- Skilled nursing visits and on-call support
- Personal care assistance (bathing, grooming)
- Medical equipment and supplies
- Medication management for comfort
- Emotional and spiritual support
- Caregiver training and respite guidance
To learn more about practical help at home, see our resources on equipment and supplies: https://www.transitionshc.com/equipment-supplies
How to decide this spring: 5 practical questions to guide your next step
During spring, routines shift—kids’ schedules change, travel plans appear, and warmer weather can make mobility or fatigue challenges more noticeable. Use these questions to get clarity when comparing palliative care vs hospice care.
1) What are the biggest “hard days” right now?
Write down the top 3 burdens:
- uncontrolled pain
- shortness of breath
- repeated ER visits
- falls or safety concerns
- caregiver burnout
- anxiety, depression, or isolation
Then ask: Which program can respond quickly and consistently to these problems where we live?
2) Are hospital visits helping—or harming quality of life?
A pattern of repeated hospitalizations can be a sign that the body is struggling to recover. Many families choose hospice care when the goal becomes comfort at home and fewer disruptive transitions.
3) What does the patient want most this season?
Some common priorities:
- staying at home
- sleeping through the night
- less pain or nausea
- being able to attend a family gathering
- maintaining dignity and independence
If you haven’t had a values-based conversation yet, a structured tool can help. Consider reviewing Five Wishes for guidance: https://www.transitionshc.com/five-wishes
4) Do caregivers have enough support to make this sustainable?
Caregiving often intensifies quickly. If the main caregiver is exhausted, missing work, or unsure how to manage symptoms, additional clinical support can make a major difference.
5) Are you unsure, but don’t want to wait until a crisis?
You don’t have to decide everything at once. A helpful first step is getting your questions answered by a care team and understanding what’s available. Many common concerns are addressed here: https://www.transitionshc.com/faqs
What care can look like: real-world examples (palliative care vs hospice)
Seeing scenarios can make palliative care vs hospice feel less abstract.
Scenario A: Advanced COPD with frequent flare-ups
- Palliative care approach: helps manage shortness of breath, anxiety, medication side effects, and advance care planning while the patient continues disease-directed therapies.
- Hospice care approach: if the patient wants to avoid repeated hospital trips and focus on comfort, hospice care can provide home-based symptom management, caregiver coaching, and 24/7 support for urgent needs.
Scenario B: Cancer with changing treatment goals
- Palliative care approach: supports pain control, appetite issues, sleep, and emotional well-being during treatment.
- Hospice care approach: if the patient decides to stop chemotherapy and prioritize quality time at home, hospice care can help stabilize symptoms, support family caregivers, and coordinate supplies and medications.
Scenario C: Dementia and increasing care needs
- Palliative care approach: addresses agitation, sleep disruption, caregiver stress, and planning for future decisions.
- Hospice care approach: when decline progresses (e.g., infections, weight loss, reduced mobility), hospice care can provide additional layers of support at home and guidance on what to expect.
Preparing for your next conversation: what to ask the doctor or care team
When families compare palliative care vs hospice, the most helpful discussions are specific. Bring these questions to an appointment:
Questions about eligibility and timing
- “Based on what you’re seeing, would palliative care help now?”
- “Could hospice care be appropriate in the next six months if things continue this way?”
- “What changes would signal it’s time to revisit hospice?”
Questions about day-to-day support
- “Who do we call after hours if symptoms spike?”
- “What equipment might help with safety and comfort at home?”
- “How will you support family caregivers?”
Questions about emotional and spiritual support
Serious illness affects the whole family. Ask:
- “Do we have access to grief and counseling resources?”
- “Is spiritual support available in a way that respects our beliefs?”
If you’re exploring grief support, you can learn more about bereavement services here: https://www.transitionshc.com/bereavement
A simple takeaway for spring decisions
If you’re deciding between palliative care vs hospice care, remember:
- Palliative care supports comfort and quality of life at any stage—often alongside treatment.
- Hospice care supports comfort-focused care when treatment goals change and home-based support becomes essential.
The right choice is the one that matches your family’s priorities this spring: fewer crises, better symptom control, and more meaningful time together.
If you’d like to talk through your situation and options, visit https://www.transitionshc.com/contact.

